Preparing for a Pandemic
Columbia University professor training nurses and students caring for COVID-19 patients

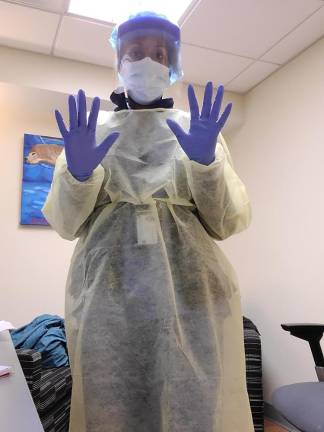
As the executive director of the simulation center at Columbia University's School of Nursing, Kellie Bryant’s job has always been to prepare students for real life scenarios that play out in hospitals every day. During the coronavirus outbreak, Bryant’s job remains the same, but the scenarios she’s prepping these students to encounter represent a new and ever-changing reality of working in the epicenter of a global pandemic.
During this time, Bryant has been tasked with both prepping nurses who have been redeployed within their hospitals to care for COVID-19 patients as well as continue to find ways to run simulations for Columbia’s nursing students, many of whom have enlisted as nurse technicians to aid in the fight against the virus.
As soon as the outbreak hit New York, Bryant and her colleagues wanted to ensure that her students had to information they needed to properly protect themselves.
“The first thing we did was offer some online modules on COVID and how to put on [Personal Protective Equipment] for students because we knew some students would be working in the hospital in their regular jobs,” said Bryant. “How do you put on the mask? How do you take it off? How do you put on a gown? What order does it go in? So we offered those classes about three times a week in the beginning.”
At New York-Presbyterian Hospital, Bryant has been helping facilitate patient simulation sessions to assist operating room nurses prepare to be redeployed to COVID-19 units.
“We would go in there and help them train the [operating room] nurses, for example, on health assessments, help them train on how to get medications and IVs because that wasn't part of their normal job requirement,” said Bryant.
Through this work, Bryant also helped the hospital adapt certain procedures and protocols for COVID-19 patients.
“When you have someone who has cardiac arrest and COVID, the way you resuscitate them is totally different. Our fear is that when you're intubating, the procedure can cause the COVID to release in the air, and it puts the health care providers at a huge risk,” said Bryant. “So my first simulation was really working with the hospital and the rapid response team to figure out how can we safely do a code where we can help save their lives and minimize the risk of COVID to the people that are in the room?”
Typically, Bryant said, when a patient is in cardiac arrest, an entire team of nurses and doctors rushes into the room with a crash cart to resuscitate the patient. But now, nurses are keeping the crash cart outside of the room and passing the supplies like a defibrillator to a limited number of people inside working on the patient. Bryant and her team practiced the new protocol through simulation, made tweaks until they felt like it could be carried through in a real life scenario.
“That was that was simulation at its best: taking a policy procedure and testing it out in simulation so that we make sure that it's up to par and the best it could be before it's really implemented in the hospital,” said Bryant. “So that was the first simulation I did once COVID came.”
Health Barriers and Racial Bias
In addition to preparing students for the technical skills they need, Bryant said the school of nursing has been providing help with the emotional impact with a program called Circle of Care.
“They're seeing unfortunately a lot of patients die,” said Bryant. “[Educators] host these meetings where students can log in and they could just talk freely about how they're feeling and kind of decompress about some of the things they're seeing.”
Bryant, who is African American, has been tasked with leading a subgroup for students of color to talk about the health barriers and racial bias as the outbreak has disproportionately impacted communities of color.
Another great challenge for Bryant in adapting simulations and teaching material to fit the coronavirus is the unpredictable nature of the virus and the various ways it manifests in patients.
“The most important thing is that we as nursing educators putting scenarios together, we got to make sure that we have the latest information. From a month ago to now, things have changed; the things that we knew about the virus has changed,” said Bryant.
She said she is part of a listserv of all simulation and medical providers throughout the country that is constantly being updated with new information, scenarios, videos and protocols. Bryant sifts through all of this to see what best fits Columbia’s policies.
“We look at all that and then we put together the best simulation based on the most recent findings,” said Bryant.
Changes for the Future
Bryant said that she has not been fully able to look to the future and think about how this pandemic will change medical procedures in the future.
“We’re still in the thrust of it,” she said. “We’re just trying to keep our heads afloat.
But she noted that a day will come where she and other educators and medical professionals will debrief and figure out how to prepare if there is another pandemic of this scale.
“It's hard to mimic exactly what would happen. It would take such a grand scheme, but maybe on a smaller scale, would could kind of rehash it and see, what are we going to implement?” said Bryant. “What are those guidelines that we need in place? We're going to have new rules because I don't I don't know if we'll ever go back to normal. I think there's always be, you know, for a while we're gonna have to wear gloves. We might still have to limit how many students are in the room. The way that we clean our equipment and supplies will probably change.”
In the meantime, Bryant said she and her fellow nurses will continue to answer the call to help patients, even though it puts them at tremendous risk.
“Even though we're stepping up to the front lines, trust me we're scared,” she said. “I think my desire to help is more than my fear.”
"From a month ago to now, things have changed; the things that we knew about the virus has changed.” Kellie Bryant